The Peritoneal Cancer Index, known as PCI, is a tool used in surgical oncology to evaluate the extent of disease within the abdominal cavity.
It is a key system in the assessment of patients with peritoneal carcinomatosis, as it allows the tumor burden to be estimated and guides therapeutic decisions, especially when considering cytoreductive surgery combined with HIPEC.
What the PCI measures
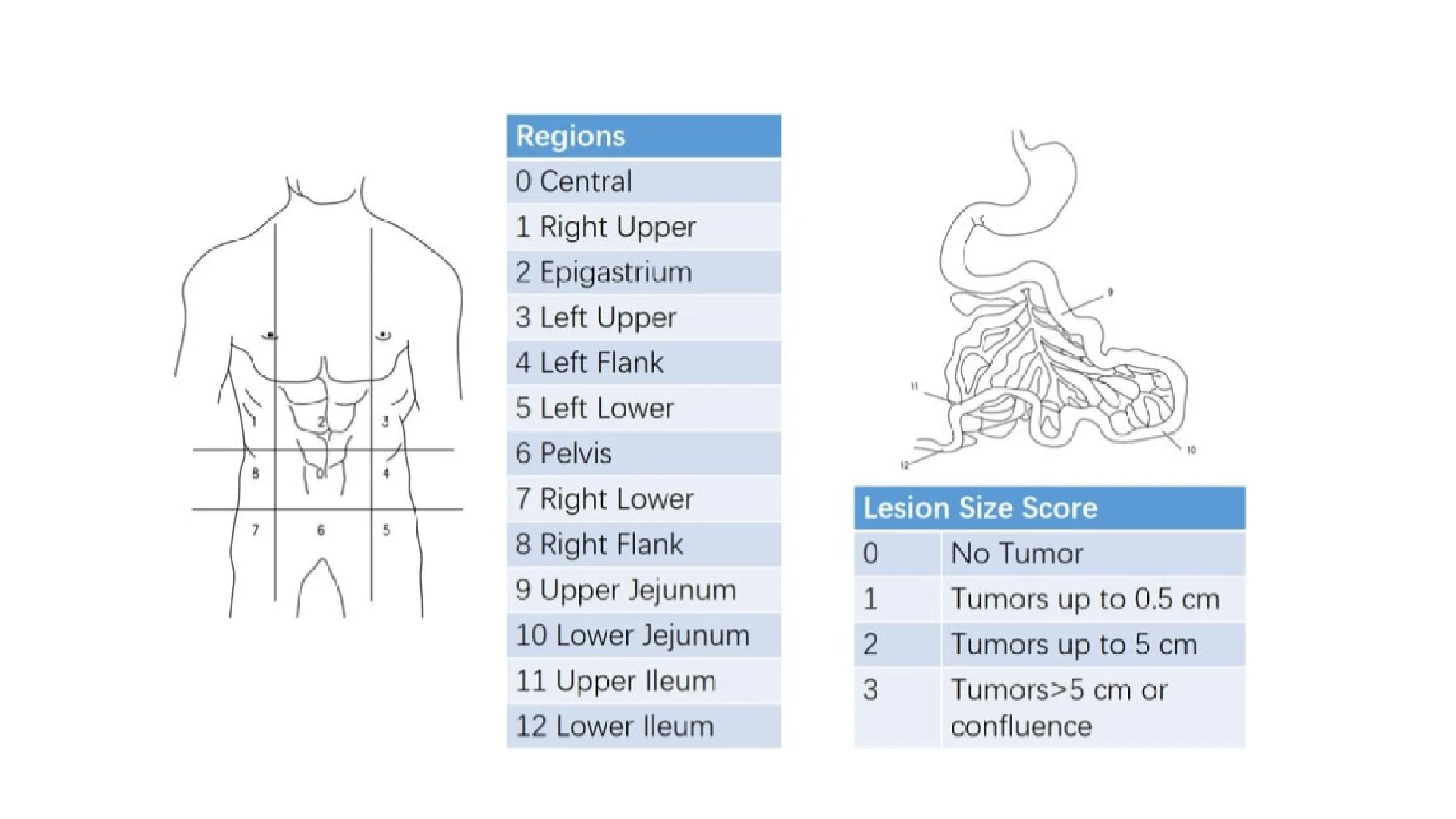
The PCI quantifies the distribution and size of tumor implants on the peritoneum. To do this, the abdomen is divided into different regions, and the presence of tumor is assessed in each one.
Each area is assigned a score based on the size of the lesions observed. The sum of these scores produces a total value that reflects the overall extent of the disease.
The higher the PCI, the greater the tumor burden.
How it is calculated
The PCI is usually calculated during surgery or, in selected cases, through imaging tests. The abdomen is divided into 13 regions, including central areas and small-bowel segments.
Each region is scored according to tumor size:
• No visible lesions — score 0
• Small nodules (less than 0.5 cm) — score 1
• Intermediate-sized lesions (between 0.5 and 5 cm) — score 2
• Large or confluent tumor implants (larger than 5 cm) — score 3
The total sum can reach high values, which indicates extensive peritoneal involvement.
What it is used for in clinical practice
The PCI is a fundamental tool to determine whether a patient can benefit from certain treatments, especially cytoreductive surgery.
In general, lower values are associated with better surgical outcomes, whereas a high PCI may indicate that the disease is too extensive for effective resection.
The index also helps standardize evaluation across different medical teams and facilitates treatment planning.
Relationship with cytoreductive surgery
One of the main uses of the PCI is to assess surgical feasibility. The possibility of removing most of the tumor in some types of cancer largely depends on the extent of the disease.
Although there is no single cut-off applicable to all cases, the PCI is one of the factors considered when selecting patients eligible for this type of intervention, together with techniques such as HIPEC.
Limitations of the index
Despite its usefulness, the PCI is not the only factor that determines treatment. Other aspects — such as tumor type, the patient's general condition or response to previous treatments — are also decisive.
For this reason, its interpretation must always be made within the context of a comprehensive clinical assessment.
Importance of specialized evaluation
Calculating and interpreting the PCI requires experience in peritoneal carcinomatosis. Its correct application allows treatment decisions to be better guided and offers a more personalized approach.
Assessment by specialized teams is key to integrating this index into the overall treatment plan.
PCI across different types of peritoneal carcinomatosis
PCI interpretation depends on the primary tumor. Each pathology has different thresholds and surgical strategies:
• Carcinomatosis of colorectal origin — low-to-moderate PCI as a selection criterion for surgery.
• Carcinomatosis of ovarian origin — tolerates higher PCI due to its chemosensitivity.
• Carcinomatosis of gastric origin — strict selection with low PCI and complete cytoreduction.
• Peritoneal pseudomyxoma (appendicular origin) — higher PCI values are accepted given its slow progression and treatment response.
• Peritoneal mesothelioma — individualized decision within a multidisciplinary committee.
Related procedures
After PCI assessment, the surgical and oncological options for eligible cases include:
• Cytoreductive surgery (CRS) — the foundational treatment to remove visible disease.
• HIPEC (hyperthermic intraperitoneal chemotherapy) — heated chemotherapy within the cavity after cytoreduction.
• PIPAC — for patients not eligible for radical surgery.
• Robotic surgery — for laparoscopic PCI assessment and selected cases.
Do you have a diagnosis of peritoneal carcinomatosis? At Quenet Torrent Institute we are a reference unit for cytoreductive surgery and HIPEC. We can review your case and calculate your PCI individually. Request an assessment.